|
press  above to
begin the lecture above to
begin the lecture
return to Pharmacology Table
of Contents
Table
of Contents
-
ß2 selective adrenergic
agonists
-
a-Selective
Adrenergic Agonists
-
a2
Selective
Adrenergic Agonists
-
Introduction
-
Clonidine
(Catapres)
-
Guanfacine
(Tenex)
-
Guanabenz
(Wytensin)
-
a-methyl DOPA
(Aldomet)
-
Miscellaneous
Amphetamine
-
Clinical Use of Sympathomimetic
Agents
|
-
Amphetamines
-
Adrenergic
Neuronal Blocking Drugs
-
Classification of
adrenoceptors (
a1, a2,ß1,
ß2
and D1), molecular consequences of their
activation, and their important locations.
-
Catecholamine
Metabolic Transformations
-
Pulmonary
Uptake
-
Adrenergic
and Cholinergic Effects on End Organs
-
Clinical
Uses: Sympathomimetic Drugs: a/b Adrenergic Agonists
-
Therapeutic
Uses of Indirect-Acting Adrenergic Agonists
-
Adverse
Effects: b Adrenergic Antagonists
-
a-Adrenergic
Antagonists
-
Introduction
-
a1-adrenergic
receptor antagonists
-
a2-adrenergic receptor antagonists
-
Phenoxybenzamine
(Dibenzyline)
-
Phentolamine(Regitine)
and tolazoline (Priscoline)
-
Prazosin
(Minipress) and Terazosin (Hytrin)
-
Others
-
b Adrenergic
Antagonists
-
Introduction
-
ß receptor blockers: Effects
on the heart
-
ß receptor blockers:
Antihypertensive
Effects
-
Pulmonary
Effects
-
Metabolic
Actions
-
Nonselective-ß adrenergic
receptor antagonists
-
propranolol
-
nadolol
-
timolol
-
labetalol
-
Cardioselective ß1 adrenergic
receptor antagonists
-
metoprolol
-
esmolol
-
atenolol
-
Adverse Effects of ß
adrenergic
receptor antagonists
-
Therapeutic
Uses
|
ß2
Selective Adrenergic Agonists
-
At low
concentration ß2
selective adrenergic agonists have relatively
minor ß1 cardiac receptor-mediated
effects.
-
Effective in managing
asthma, ß2 selective adrenergic
agonists are orally active and metabolized more
slowly compared to catecholamines
ß2 selective adrenergic agonists
|
metaproterenol
(Alupent)
|
terbutaline
(Brethine)
|
albuterol
(Ventolin,Proventil)
|
-
In asthma, pulmonary ß2
receptors are targeted by drug administration by
inhalation.
-
Activation of pulmonary ß2
adrenergic receptors result in smooth-muscle relaxation and bronchodilation.
-
ß adrenergic
receptor agonists also decrease histamine and
leukotriene release from lung mast cells.
Recalling that asthma is first and foremost an
inflammatory disease, reduction in histamine and
leukotriene release would be beneficial.
-
ß adrenergic
receptor agonists enhance mucociliary activity
and diminish microvascular permeabilty.
return to Table of Contents
Metaproterenol
(Alupent)
-
ß2 adrenergic
receptor-selective: resistant to COMT (catechol-O-methyl
transferase) metabolism
-
Less ß2 selective
compared to terbutaline (Brethine) and albuterol (Ventolin,Proventil).
-
May be used for long-term and
acute treatment of bronchospasm
return to Table of Contents
Terbutaline [Brethine]
-
ß2 adrenergic
receptor-selective: resistant to COMT
-
Active after oral, subcutaneous,
or administration by inhalation
-
Rapid onset of action.
-
Used for management of
chronic obstructive lung disease and for
treatment of acute bronchospasm (smooth muscle
bronchoconstriction), including status
asthmaticus
Albuterol [Ventolin]
-
ß2 adrenergic
receptor-selective
-
Effective following
inhalation or oral administration.
-
Commonly used in chronic
and acute asthma management.
Ritodrine
(Yutopar)
-
ß2 adrenergic
receptor-selective: developed as a uterine
relaxant
-
May be administered by i.v. in
certain patients for arresting premature labor;
if successful, oral therapy may be started.
-
ß2 adrenergic
receptor-selective agonists may not improve
perinatal mortality and may increase maternal
morbidity.
-
In women being treated for
premature labor, ritodrine (Yutopar) or
terbutaline (Brethine) may cause pulmonary edema
.
return to Table of Contents
Adverse Effects-Agonists
-
Excessive
cardiovascular stimulation
-
Skeletal
muscle tremor (tolerance develops, unknown
mechanism) due to ß2 adrenergic
receptor activation
-
Overusage
may be a factor in morbidity and mortality in
asthmatics.

Hoffman,
B.B and Lefkowitz, R.J, Catecholamines, Sympathomimetic
Drugs, and Adrenergic Receptor Antagonists, In, Goodman
and Gillman's The Pharmacologial Basis of Therapeutics,
(Hardman, J.G, Limbird, L.E, Molinoff, P.B., Ruddon, R.W,
and Gilman, A.G.,eds) TheMcGraw-Hill Companies,
Inc.,1996, pp.213-216.
return to Table of Contents
Alpha1
Selective Adrenergic Agonists
-
Smooth muscle tone is determined
by modulation of myosin light-chain kinase
activation.
-
Myosin light-chain kinase
phosphorylates myosin--a step that
initiates myosin-actin interaction. (by
contrast in skeletal or cardiac muscle Ca2+
interaction with troponin is central to
initiation of muscle contraction)
-
Increases in intracellular
Ca2+ with Ca2+
calmodulin complex formation results in
activation of myosin light-chain kinase.
-
alpha1 receptor
activation causes Ca2+ influx
-
In some cells, a1
receptor activation causes
IP3 production, which releases
sequested Ca2+.
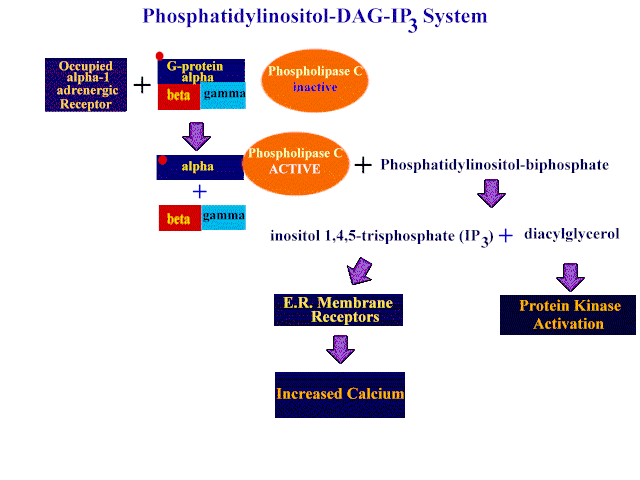
return to Table of Contents
Methoxamine
(Vasoxyl)
-
specific alpha1
receptor agonist
-
increases peripheral
resistance
-
causes an increase in
blood pressure that precipitates sinus
bradycardia (decreased heart rate) due to vagal
reflex.
-
Reflex bradycardia may be
block by atropine (muscarinic antagonist)
Clinical use:
Phenylephrine
(Neo-Synephrine)
-
Specific alpha1
receptor agonist
-
Increases peripheral
resistance
-
Causes an increase in
blood pressure that precipitates sinus
bradycardia (decreased heart rate) due to vagal
reflex.
-
Reflex bradycardia may be
block by atropine (muscarinic antagonist)
-
Clinical use:
-
hypotensive states
-
mydriatic
-
nasal decongestant
return to Table of Contents
Hoffman, B.B and Lefkowitz, R.J, Catecholamines, Sympathomimetic Drugs, and Adrenergic
Receptor Antagonists, In, Goodman and Gillman's The
Pharmacologial Basis of Therapeutics,(Hardman, J.G, Limbird, L.E,
Molinoff, P.B., Ruddon, R.W, and Gilman, A.G.,eds) TheMcGraw-Hill Companies, Inc.,1996,
pp.216-219.
alpha2
Selective Adrenergic Agonists and Miscellaneous Adrenergic Agonists
Introduction
Clonidine
(Catapres)
-
Clonidine (Catapres) is primarily used in treating essential hypertension.
-
A prolonged hypotensive response
results from a decrease in CNS sympathetic
outflow.
-
This response is due to a2
selective adrenergic
receptor activation.{Vertebral arterial or intra
cisterna magna injection results in hypotension.
This experiment demonstrate clonidine central
action.}
Adverse Effects:
-
dry mouth
-
sedation
-
sexual
dysfunction
Guanabenz
Wytensin)
-
Guanabenz (Wytensin)is primarily used in treating essential hypertension.
-
A prolonged hypotensive response
results from a decrease in CNS sympathetic
outflow.
-
This response is due to a2
selective adrenergic
receptor activation.
Adverse Effects:
Guanfacine
-
Guanfacine is
used for treating essential hypertension.
-
A prolonged hypotensive response
results from a decrease in CNS sympathetic
outflow.
-
This response is due to a2
selective adrenergic
receptor activation. a2
receptor selectivity is
greater than that observed with clonidine despite
similar efficacy in treating hypertension.
-
Adverse Effects:
Alpha-methyl DOPA--
(methyldopa (Aldomet))
-
Alpha-methyl DOPA (methyldopa (Aldomet)), metabolically
converted to alpha-methyl norepinephrine, is used
for treating essential hypertension.
-
A prolonged hypotensive response
results from a decrease in CNS sympathetic
outflow.
-
This response is due to a2
selective adrenergic
receptor activation.
Adverse Effects:
Amphetamine
-
CNS stimulant (releasing biogenic nerve
terminal amines:
-
Other
effects: headache, palpitations, dysphoria
-
Indirect acting sympathomimetic
-
Toxicity:
-
CNS: restlessness, tremor,
irritablity, insomnia, aggressiveness,
anxiety, panic, suicidal ideation, etc.
-
Cardiovascular:
arrhythmias, hypertension or hypotension,
angina
-
GI: dry mouth, anorexia,
vomiting, diarrhea, cramping
-
Treatment:
-
urinary
acidification by ammonium
chloride
-
hypertension:
nitroprusside or a adrenergic receptor
antagonist
-
CNS:
sedative-hypnotic drugs
-
Therapeutic Use:
Methylphenidate (Ritalin)
-
Mild CNS stimulant, chemically
related to amphetamine
-
Effects more prevalent on mental
than motor activities
-
General pharmacological profile
similar to amphetamine
-
Major
Therapeutic Use:
Ephedrine
-
alpha and
ß adrenergic receptor agonist
-
Indirect
sympathomimetic also, promoting norepinephrine
release
-
non-catechol structure, orally
active
-
Pharmacological effects:
-
increases heart rate,
cardiac output
-
usually increases blood
pressure
-
may cause uriniary
hesitancy due to stimulation of a smooth muscle receptors in
bladder base.
-
bronchodilation: ß
adrenergic receptor response
-
Limited Clinical Use due to better
pharmacological alternatives (asthma, heart
block, CNS stimulation)
return to Table of Contents
Hoffman, B.B and Lefkowitz, R.J, Catecholamines, Sympathomimetic Drugs, and Adrenergic
Receptor Antagonists, In, Goodman and Gillman's The
Pharmacologial Basis of Therapeutics, (Hardman, J.G, Limbird, L.E,
Molinoff, P.B., Ruddon, R.W, and Gilman, A.G.,eds) TheMcGraw-Hill Companies, Inc.,1996,
pp.216-219
Amphetamine
& related drugs
-
use (very limited) as appetite suppressant with
high abuse potential
-
Fenfluramine: appetite suppressant; cardiotoxic (withdrawn
from market)
-
Methylphenidate (Ritalin)
similar but with fewer peripheral
effects, useful in Attention Deficit
Disorder
return to Table of
Contents
press the purple
arrow below (right) to go to the next page
|