Owen MJ, Sawa A, Mortensen PB.
Schizophrenia. Lancet. 2016;388(10039):86–97. doi:
10.1016/S0140-6736(15)01121-6.
https://pubmed.ncbi.nlm.nih.gov/26777917/
Lichtenstein P, Yip BH, Björk C, et al.. Common
genetic determinants of schizophrenia and bipolar
disorder in Swedish families: a population-based
study. Lancet. 2009;373(9659):234–239. doi:
10.1016/S0140-6736(09)60072-6.
https://pubmed.ncbi.nlm.nih.gov/19150704/
Cross-Disorder Group of the Psychiatric Genomics
Consortium. Genetic relationship between five
psychiatric disorders estimated from genome-wide
SNPs. Nat Genet. 2013;45(9):984–994. doi:
10.1038/ng.2711.
https://pubmed.ncbi.nlm.nih.gov/23933821/
van Os J, Kapur S. Schizophrenia. Lancet.
2009;374(9690):635–645. doi:
10.1016/S0140-6736(09)60995-8.
https://pubmed.ncbi.nlm.nih.gov/19700006/
Goodwin FK, Jamison KR. Manic-Depressive Illness:
Bipolar Disorders and Recurrent Depression (2nd
ed.). Oxford University Press. 2007. ISBN:
978-0195135794.
https://global.oup.com/academic/product/manic-depressive-illness-9780195135794
Keck PE Jr, McElroy SL, Havens JR, et al..
Psychosis in bipolar disorder: phenomenology and
impact on morbidity and course of illness. Compr
Psychiatry. 2003;44(4):263–269. doi:
10.1016/S0010-440X(03)00080-2.
https://pubmed.ncbi.nlm.nih.gov/12923706/
Menezes NM, Arenovich T, Zipursky RB. A
systematic review of longitudinal outcome studies of
first-episode psychosis. Psychol Med.
2006;36(10):1349–1362. doi:
10.1017/S0033291706007951.
https://pubmed.ncbi.nlm.nih.gov/16756689/
Perkins DO, Gu H, Boteva K, Lieberman JA.
Relationship between duration of untreated psychosis
and outcome in first-episode schizophrenia: a
critical review and meta-analysis. Am J Psychiatry.
2005;162(10):1785–1804. doi:
10.1176/appi.ajp.162.10.1785.
https://pubmed.ncbi.nlm.nih.gov/16199825/
Ventura J, Subotnik KL, Nuechterlein KH. Negative
symptoms are the predominant predictor of functional
impairment in the early course of schizophrenia.
Schizophr Res. 2009;107(1):13–19. doi:
10.1016/j.schres.2008.09.026.
https://pubmed.ncbi.nlm.nih.gov/18986795/
Harding CM, Brooks GW, Ashikaga T, et al.. The
Vermont longitudinal study of persons with severe
mental illness, I: Methodology, study sample, and
overall status 32 years later. Am J Psychiatry.
1987;144(6):718–726. doi: 10.1176/ajp.144.6.718.
https://pubmed.ncbi.nlm.nih.gov/3591988/
Penttilä M, Jääskeläinen E, Hirvonen N, et al..
Duration of untreated psychosis as predictor of
long-term outcome in schizophrenia: systematic
review and meta-analysis. Br J Psychiatry.
2014;205(2):88–94. doi: 10.1192/bjp.bp.113.127753.
https://pubmed.ncbi.nlm.nih.gov/25252316/
Penttilä M, Jääskeläinen E, Hirvonen N, et al..
Duration of untreated psychosis as predictor of
long-term outcome in schizophrenia: systematic
review and meta-analysis. Br J Psychiatry.
2014;205(2):88–94. doi: 10.1192/bjp.bp.113.127753.
https://pubmed.ncbi.nlm.nih.gov/25252316/
Kirkpatrick B, Fenton WS, Carpenter WT Jr, Marder
SR. The NIMH-MATRICS consensus statement on negative
symptoms. Schizophr Bull. 2006;32(2):214–219. doi:
10.1093/schbul/sbj053.
https://pubmed.ncbi.nlm.nih.gov/16481659/
Saha S, Chant D, McGrath J. A systematic review
of mortality in schizophrenia: is the differential
mortality gap worsening over time?. Arch Gen
Psychiatry. 2007;64(10):1123–1131. doi:
10.1001/archpsyc.64.10.1123.
https://pubmed.ncbi.nlm.nih.gov/17909124/
Mitchell AJ, Vancampfort D, Sweers K, et al..
Prevalence of metabolic syndrome and metabolic
abnormalities in schizophrenia and related
disorders: a systematic review and meta-analysis.
Schizophr Bull. 2013;39(2):306–318. doi: 10.1093/schbul/sbr148.
https://pubmed.ncbi.nlm.nih.gov/22207632/
Pompili M, Gonda X, Serafini G, et al..
Epidemiology of suicide in bipolar disorders: a
systematic review of the literature. Bipolar Disord.
2013;15(5):457–490. doi: 10.1111/bdi.12087.
https://pubmed.ncbi.nlm.nih.gov/23755739/
Tohen M, Hennen J, Zarate CM Jr, et al.. Two-year
syndromal and functional recovery in 219 cases of
first-episode major affective disorder with
psychotic features. Am J Psychiatry.
2000;157(2):220–228. doi:
10.1176/appi.ajp.157.2.220.
https://pubmed.ncbi.nlm.nih.gov/10671390/
Ketter TA, Calabrese JR. Stabilization of mood
from below versus above baseline in bipolar
disorder: a new nomenclature. J Clin Psychiatry.
2002;63(2):146–151. doi: 10.4088/jcp.v63n0208.
https://pubmed.ncbi.nlm.nih.gov/11874217/
Judd LL, Akiskal HS, Schettler PJ, et al.. The
long-term natural history of the weekly symptomatic
status of bipolar I disorder. Arch Gen Psychiatry.
2002;59(6):530–537. doi: 10.1001/archpsyc.59.6.530.
https://pubmed.ncbi.nlm.nih.gov/12044195/
Miklowitz DJ, Otto MW, Frank E, et al..
Psychosocial treatments for bipolar depression: a
1-year randomized trial from the Systematic
Treatment Enhancement Program. Arch Gen Psychiatry.
2007;64(4):419–426. doi: 10.1001/archpsyc.64.4.419.
https://pubmed.ncbi.nlm.nih.gov/17404119/
Hayes JF, Marston L, Walters K, et al.. Mortality
gap for people with bipolar disorder and
schizophrenia: UK-based cohort study 2000–2014. Br J
Psychiatry. 2017;211(3):175–181. doi:
10.1192/bjp.bp.117.202606.
https://pubmed.ncbi.nlm.nih.gov/28684404/
Yatham LN, Kennedy SH, Parikh SV, et al.. CANMAT
and ISBD 2018 guidelines for the management of
patients with bipolar disorder. Bipolar Disord.
2018;20(2):97–170. doi: 10.1111/bdi.12609.
https://pubmed.ncbi.nlm.nih.gov/29536616/
Andreasen NC, Carpenter WT Jr, Kane JM, et al..
Remission in schizophrenia: proposed criteria and
rationale for consensus. Am J Psychiatry.
2005;162(3):441–449. doi:
10.1176/appi.ajp.162.3.441.
https://pubmed.ncbi.nlm.nih.gov/15741458/
Heinrichs RW, Zakzanis KK. Neurocognitive deficit
in schizophrenia: a quantitative review of the
evidence. Neuropsychology. 1998;12(3):426–445. doi:
10.1037/0894-4105.12.3.426.
https://pubmed.ncbi.nlm.nih.gov/9673998/
Mesholam-Gately RI, Giuliano AJ, Goff KP, et al..
Neurocognition in first-episode schizophrenia: a
meta-analytic review. Neuropsychology.
2009;23(3):315–336. doi: 10.1037/a0014708.
https://pubmed.ncbi.nlm.nih.gov/19413443/
Goldman-Rakic PS. Working memory dysfunction in
schizophrenia. J Neuropsychiatry Clin Neurosci.
1994;6(4):348–357. doi: 10.1176/jnp.6.4.348.
https://pubmed.ncbi.nlm.nih.gov/7841806/
Green MF, Kern RS, Braff DL, Mintz J.
Neurocognitive deficits and functional outcome in
schizophrenia: are we measuring the 'right stuff'?.
Schizophr Bull. 2000;26(1):119–136. doi:
10.1093/oxfordjournals.schbul.a033430.
https://pubmed.ncbi.nlm.nih.gov/10755673/
Bora E, Murray RM. Meta-analysis of cognitive
deficits in ultra-high risk to psychosis and
first-episode psychosis: do the cognitive deficits
progress over, or after, the onset of psychosis?.
Schizophr Bull. 2014;40(4):744–755. doi: 10.1093/schbul/sbt085.
https://pubmed.ncbi.nlm.nih.gov/23770934/
Reichenberg A, Weiser M, Rabinowitz J, et al.. A
population-based cohort study of premorbid
intellectual, language, and behavioral functioning
in patients with schizophrenia, schizoaffective
disorder, and nonpsychotic bipolar disorder. Am J
Psychiatry. 2002;159(12):2027–2035. doi:
10.1176/appi.ajp.159.12.2027.
https://pubmed.ncbi.nlm.nih.gov/12450953/
Schaefer J, Giangrande E, Weinberger DR,
Dickinson D. The global cognitive impairment in
schizophrenia: consistent over decades and around
the world. Schizophr Res. 2013;150(1):42–50. doi:
10.1016/j.schres.2013.07.009.
https://pubmed.ncbi.nlm.nih.gov/23911259/
Harvey PD, Silverman JM, Mohs RC, et al..
Cognitive decline in late-life schizophrenia: a
longitudinal study of geriatric chronically
hospitalized patients. Biol Psychiatry.
1999;45(1):32–40. doi:
10.1016/S0006-3223(98)00273-X.
https://pubmed.ncbi.nlm.nih.gov/9894574/
Keefe RS, Bilder RM, Davis SM, et al..
Neurocognitive effects of antipsychotic medications
in patients with chronic schizophrenia in the CATIE
Trial. Arch Gen Psychiatry. 2007;64(6):633–647. doi:
10.1001/archpsyc.64.6.633.
https://pubmed.ncbi.nlm.nih.gov/17548746/
Arts B, Jabben N, Krabbendam L, van Os J.
Meta-analyses of cognitive functioning in euthymic
bipolar patients and their first-degree relatives.
Psychol Med. 2008;38(6):771–785. doi:
10.1017/S0033291707001675.
https://pubmed.ncbi.nlm.nih.gov/17922938/
Bora E, Yucel M, Pantelis C. Cognitive
endophenotypes of bipolar disorder: a meta-analysis
of neuropsychological deficits in euthymic patients
and their first-degree relatives. J Affect Disord.
2009;113(1–2):1–20. doi: 10.1016/j.jad.2008.06.009.
https://pubmed.ncbi.nlm.nih.gov/18684514/
Bora E, Yucel M, Pantelis C. Cognitive
functioning in schizophrenia, schizoaffective
disorder and affective psychoses: meta-analytic
study. Br J Psychiatry. 2009;195(6):475–482. doi:
10.1192/bjp.bp.108.055731.
https://pubmed.ncbi.nlm.nih.gov/19949194/
Simonsen C, Sundet K, Vaskinn A, et al..
Neurocognitive profiles in bipolar I and bipolar II
disorder: differences in pattern and magnitude of
dysfunction. Bipolar Disord. 2008;10(2):245–255. doi:
10.1111/j.1399-5618.2007.00492.x.
https://pubmed.ncbi.nlm.nih.gov/18271904/
Hill SK, Reilly JL, Keefe RS, et al..
Neuropsychological impairments in schizophrenia and
psychotic bipolar disorder: findings from the
Bipolar-Schizophrenia Network on Intermediate
Phenotypes (B-SNIP) study. Am J Psychiatry.
2013;170(11):1275–1284. doi:
10.1176/appi.ajp.2013.12101298.
https://pubmed.ncbi.nlm.nih.gov/23771170/
Murray CJ, Lopez AD. Global mortality,
disability, and the contribution of risk factors:
Global Burden of Disease Study. Lancet.
1997;349(9063):1436–1442. doi:
10.1016/S0140-6736(96)07495-8.
https://pubmed.ncbi.nlm.nih.gov/9164317/
Green MF. What are the functional consequences of
neurocognitive deficits in schizophrenia?. Am J
Psychiatry. 1996;153(3):321–330. doi:
10.1176/ajp.153.3.321.
https://pubmed.ncbi.nlm.nih.gov/8610818/
Rosa AR, Reinares M, Michalak EE, et al..
Functional impairment and disability across mood
states in bipolar disorder. Value Health.
2010;13(8):984–988. doi:
10.1111/j.1524-4733.2010.00768.x.
https://pubmed.ncbi.nlm.nih.gov/20659274/
Cardno AG, Gottesman II. Twin studies of
schizophrenia: from bow-and-arrow concordances to
star wars Mx and functional genomics. Am J Med
Genet. 2000;97(1):12–17. doi:
10.1002/(SICI)1096-8628(200021)97.
https://pubmed.ncbi.nlm.nih.gov/10813800/
Kendler KS, McGuire M, Gruenberg AM, Walsh D.
Schizotypal symptoms and signs in the Roscommon
Family Study: their factor structure and familial
relationship with psychotic and affective disorders.
Arch Gen Psychiatry. 1995;52(4):296–303. doi:
10.1001/archpsyc.1995.03950160054009.
https://pubmed.ncbi.nlm.nih.gov/7702447/
McGuffin P, Rijsdijk F, Andrew M, et al.. The
heritability of bipolar affective disorder and the
genetic relationship to unipolar depression. Arch
Gen Psychiatry. 2003;60(5):497–502. doi:
10.1001/archpsyc.60.5.497.
https://pubmed.ncbi.nlm.nih.gov/12742871/
Angst J. The bipolar spectrum. Br J Psychiatry.
2007;190:189–191. doi: 10.1192/bjp.bp.106.030957.
https://pubmed.ncbi.nlm.nih.gov/17329735/
Bulik-Sullivan B, Finucane HK, Anttila V, et al..
An atlas of genetic correlations across human
diseases and traits. Nat Genet.
2015;47(11):1236–1241. doi: 10.1038/ng.3406.
https://pubmed.ncbi.nlm.nih.gov/26414676/
Ruderfer DM, Fanous AH, Ripke S, et al..
Polygenic dissection of diagnosis and clinical
dimensions of bipolar disorder and schizophrenia.
Mol Psychiatry. 2014;19(9):1017–1024. doi:
10.1038/mp.2013.138.
https://pubmed.ncbi.nlm.nih.gov/24105046/
Smoller JW, Kendler K, Craddock N, et al..
Identification of risk loci with shared effects on
five major psychiatric disorders: a genome-wide
analysis. Lancet. 2013;381(9875):1371–1379. doi:
10.1016/S0140-6736(12)62129-1.
https://pubmed.ncbi.nlm.nih.gov/23453885/
Niemi LT, Suvisaari JM, Tuulio-Henriksson A,
Lönnqvist JK. Childhood developmental abnormalities
in schizophrenia: evidence from high-risk studies.
Schizophr Res. 2003;60(2–3):239–258. doi:
10.1016/S0920-9964(02)00291-3.
https://pubmed.ncbi.nlm.nih.gov/12591589/
Gandal MJ, Haney JR, Parikshak NN, et al.. Shared
molecular neuropathology across major psychiatric
disorders parallels polygenic overlap. Science.
2018;359(6376):693–697. doi:
10.1126/science.aad6469.
https://pubmed.ncbi.nlm.nih.gov/29439242/
Sekar A, Bialas AR, de Rivera H, et al..
Schizophrenia risk from complex variation of
complement component 4. Nature.
2016;530(7589):177–183. doi: 10.1038/nature16549.
https://pubmed.ncbi.nlm.nih.gov/26814963/
Sekar A, Bialas AR, de Rivera H, et al..
Schizophrenia risk from complex variation of
complement component 4. Nature.
2016;530(7589):177–183. doi: 10.1038/nature16549.
https://pubmed.ncbi.nlm.nih.gov/26814963/
Kasanin J. The acute schizoaffective psychoses.
Am J Psychiatry. 1933;90(1):97–126. doi:
10.1176/ajp.90.1.97.
https://doi.org/10.1176/ajp.90.1.97
Kendler KS, Gruenberg AM, Tsuang MT. Psychiatric
illness in first-degree relatives of schizophrenic
and surgical control patients: a family study using
DSM-III criteria. Arch Gen Psychiatry.
1985;42(8):770–779. doi:
10.1001/archpsyc.1985.01790310022002.
https://pubmed.ncbi.nlm.nih.gov/4015309/
Regier DA, Narrow WE, Clarke DE, et al.. DSM-5
field trials in the United States and Canada, Part
II: test-retest reliability of selected categorical
diagnoses. Am J Psychiatry. 2013;170(1):59–70. doi:
10.1176/appi.ajp.2012.12070999.
https://pubmed.ncbi.nlm.nih.gov/23111466/
Craddock N, Owen MJ. The Kraepelinian dichotomy —
going, going... but still not gone. Br J Psychiatry.
2010;196(2):92–95. doi: 10.1192/bjp.bp.109.073429.
https://pubmed.ncbi.nlm.nih.gov/20118450/
Rimol LM, Hartberg CB, Nesvåg R, et al.. Cortical
thickness and subcortical volumes in schizophrenia
and bipolar disorder. Biol Psychiatry.
2010;68(1):41–50. doi:
10.1016/j.biopsych.2010.03.036.
https://pubmed.ncbi.nlm.nih.gov/20497902/
Turetsky BI, Calkins ME, Light GA, et al..
Neurophysiological endophenotypes of schizophrenia:
the viability of selected candidate measures.
Schizophr Bull. 2007;33(1):69–94. doi: 10.1093/schbul/sbl060.
https://pubmed.ncbi.nlm.nih.gov/17135482/

![]() In
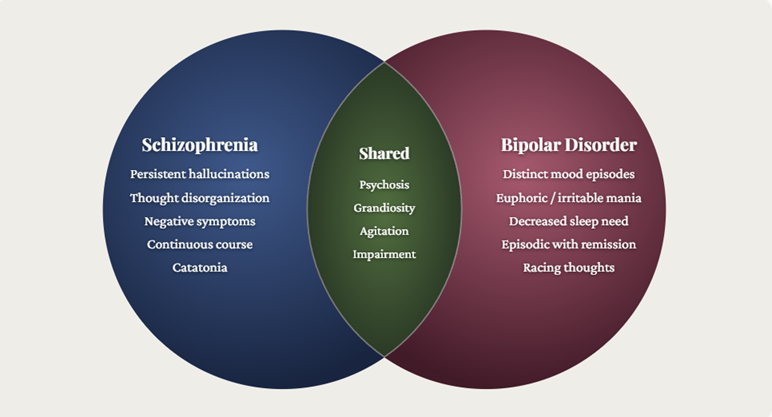
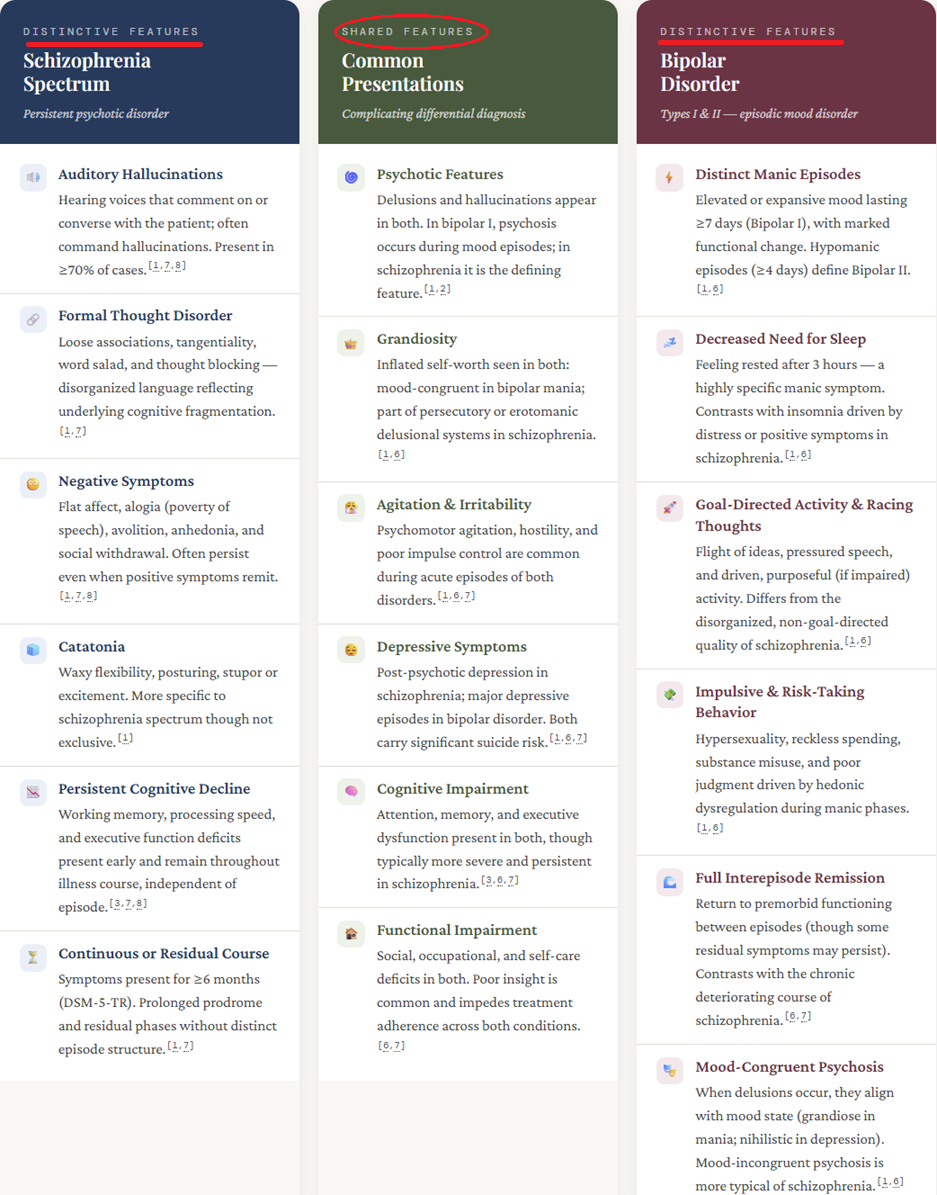
schizophrenia and schizoaffective disorder, psychotic symptoms such
as positive symptoms including hallucinations and delusions, and
disorganized thinking are defining and often primary features.
In
schizophrenia and schizoaffective disorder, psychotic symptoms such
as positive symptoms including hallucinations and delusions, and
disorganized thinking are defining and often primary features.
![]() In bipolar
disorder, psychotic features occur predominantly during acute manic
or depressive episodes.
In bipolar
disorder, psychotic features occur predominantly during acute manic
or depressive episodes.