|
|
|
Asthma: Systems Pathophysiology
Pathophysiologic Manifestations
Airway diameter reduction, caused by smooth muscle contraction, vascular congestion, bronchial wall edema and thick, tenacious secretion.
Consequences of Airway Diameter Reduction in Acute Asthma
Increased airway resistance
Decreased forced expiratory rates
Increased work of breathing
Changes in respiratory muscle function
Changes in elastic recoil
Abnormal ventilation/pulmonary blood flow distribution
Ventilation/perfusion mismatching
Lung and thorax hyperinflation
|
|
|
9Compromised pulmonary function in Asthma
ECG changes indicative of right ventricular hypertrophy and pulmonary hypertension
Vital capacity < 50% of normal
1-second forced expiratory volume (FEV1): reduced to 30% of expected
Maximum/a minimum midexpiratory flow rates: reduced to 20% or less of expected
In acute illness: residual volume (RV): may approach 400% of normal; functional residual capacity doubles
Patients report that the attack has ended clinically when RV has fallen to 200% of expected and FEV1 reaches 50% of expected level
Very common finding during acute phase
Respiratory failure -- relatively uncommon: 10% to 15% of presenting patients
Hypercapnea: common
Respiratory alkalosis: common
Normal arterial carbon dioxide tension but severe airway obstruction present is suggestive of possibly impending respiratory failure
Metabolic acidosis in acute asthma with severe obstruction
Clinical presentations may not correlate with blood gas data; however, estimating patient's ventilatory state solely on clinical presentation may be dangerous
Patients with possible alveolar hypoventilation should have arterial blood gas tension measurements
Cyanosis: -- very late sign; suggestive that extreme hypoxia may go undetected.
Some Clinical Features in Asthma
There are three principal symptoms that characterize asthma.
These are dyspnea, cough, and wheezing with wheezing being particularly prominent.
Asthma is an episodic disorder with the above symptoms commonly exhibited.
Initially patients experienced chest constriction perhaps with a nonproductive cough.
Audibly harsh, wheezing respiration is then noted; expiration is prolonged and difficult.
Tachypnea, mild systolic hypertension and tachycardia are frequent presentations.
Lung overinflation is typical in the anterioposterior thoracic dimension (diameter) increases.
Severe or prolonged asthma attacks are associated with a loss of adventitial breath sounds along with notably high pitched wheezing.
Respiratory accessory muscles become more prominent as well as paradoxical pulse-signs indicative of severe obstruction with impaired, significantly impaired pulmonary function.
Paradoxical pulse requires significantly large negative intrathoracic pressures; therefore, with shallow breathing, condition which does not favor development of large negative intrathoracic pressures, significant obstruction can be present even in the absence of paradoxical pulse.
[Paradoxical pulse definition: Inspiratory decrease in arterial pressure >10 mm Hg with Inspiratory venous pressure unchanged (Kussmaul's Sign); Paradoxical pulse signs: Palpable decrease in pulse with inspiration Inspiratory systolic blood pressure decreased over 10 mm Hg less than expiratory pressure]. Significant disease may remain if the endpoints are only an a reduction in wheezing and the resolution of subjective complaints.
The conclusion of an asthmatic episode may be associated with coughs producing a thick, stringy me at this in the form of distal airway casts (Curschmann's spirals) which when microscopically evaluated shows the presence of eosinophils and Charcot-Leyden crystals.
|
|
|
|
|
Severe mucus plugging with possibly imminent suffocation may occur and in this case the cough would be ineffective and the patient will be gasping.
Such circumstances may necessitate mechanical ventilation. Atelectasis (collapsed lung) may also occur in asthma.
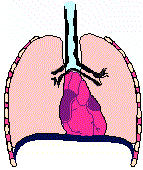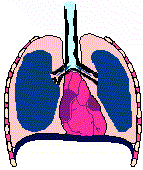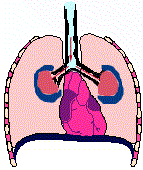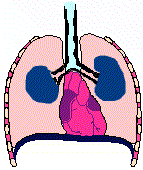
Bronchial wall characteristics during an acute asthma attack
|
|
|
Animation of asthmatic breathing cycle noting residual lung volume (copyright (C) 1996, Stephen M. Borowitz)
1 McFadden, E.R., Jr. "Asthma: Diseases of the Respiratory System" in Harrison's Principles of Internal Medicine, 15th Edition (Braunwald, E., Fauci, A.S., Kasper, D.L., Hauser, S.L, Longo, D.L. and Jameson, J. Larry, eds) pp. 1456-1463, McGraw-Hill Medical Pubishing, Division, New York, 2001
2 Kelley, H. William, "Asthma" in Pharmacotherapy: A Pathophysiologic Approach, (Dipiro, J.T., Talkbert, R.L. Yee, G.C., Matze, G.R., Wells, B.G. and Posey, L. Michael, eds.) pp 430-459. McGraw-Hill Medical Pubishing, Division, New York, 1999.
3Spencer SM., Sgro JY., Dryden KA., Baker TS., Nibert ML. (1997) Rhinovirus 14 (3D image reconstruction from electron microscopy data) Journal of Structural Biology. 120(1):11-21
4Attribution: Michigan State University Website:
5State University of New York, Upstate Medical University, Cytotechnology, On-Line Courseware,
6Steve Dewhurst, Ph.D., Structure of the CC-chemokine, RANTES, (c) University of Rochester and Stephen Dewhurst, 1999
7Ealick SE, Recombinant Human Granulocyte-Macrophage Colony-Stimulating Factor, Cornell University
Walter MR, Cook WJ, Ealick SE, Nagabhushan, TL, Trotta, PP and Bugg, CE. Three-Dimensional Structure of Recombinant Human Granulocyte-Macrophage Colony-Stimulating Factor, J. Mol. Biol. 224:1075-1085 (1992).
Reichert P, Ealick SE, Cook WJ, Trotta P, Nagabhushan TL, Bugg CE. Crystallization and Preliminary X-ray Investigation of Human Granulocyte-Macrophage Colony Stimulating Factor, J. Biol. Chem. 265(1):452-453 (1990)
8Williams, TJ and Conroy, TM Eotaxin and the attraction of eosinophils to the asthmatic lung, Respir Res 2001, 2: 150-156
9McFadden, Jr., E. R., Diseases of the Respiratory System: Asthma, In Harrison's Principles of Internal Medicine 14th edition, (Isselbacher, K.J., Braunwald, E., Wilson, J.D., Martin, J.B., Fauci, A.S. and Kasper, D.L., eds) McGraw-Hill, Inc (Health Professions Division), 1998, p 1422.
10Daroca, P, Lung and Respiratory System
Review, Tulane University Pathology, (Figure & caption
attribution)
|
This Web-based pharmacology and disease-based integrated teaching site is based on reference materials, that are believed reliable and consistent with standards accepted at the time of development. Possibility of human error and on-going research and development in medical sciences do not allow assurance that the information contained herein is in every respect accurate or complete. Users should confirm the information contained herein with other sources. This site should only be considered as a teaching aid for undergraduate and graduate biomedical education and is intended only as a teaching site. Information contained here should not be used for patient management and should not be used as a substitute for consultation with practicing medical professionals. Users of this website should check the product information sheet included in the package of any drug they plan to administer to be certain that the information contained in this site is accurate and that changes have not been made in the recommended dose or in the contraindications for administration. Advertisements that appear on this site are not reviewed for content accuracy and it is the responsibility of users of this website to make individual assessments concerning this information. Medical or other information thus obtained should not be used as a substitute for consultation with practicing medical or scientific or other professionals. |