|
press  above to
begin the lecture above to
begin the lecture
and
install current free versions of Quicktime,
if needed, to support lecture series audio!
-
Absorption
-
Routes of
Administration
-
First-Pass Effect
-
Pulmonary
Effects
-
Pharmacokinetics
|
-
Drug
Metabolism
-
Introduction
-
Phase
I and Phase II Reaction Overview:
-
Phase
I characteristics
-
Phase
II characteristics
-
Conjugates
-
Principal
organs for biotransformation
-
Bioavailability
-
Microsomal
Mixed Function Oxidase System and Phase I Reactions
-
Phase II Reactions
-
Individual
Variation in Drug Responses
-
Genetic
Factors in Biotransformation
-
Effects
of Age on Drug Responses
-
Drug-Drug
Interactions
Pharmacokinetics
and some IV Anesthetics Agents
-
Barbiturates
-
Benzodiazepines
-
Ketamine
and Etomidate
-
Propofol
-
Opioids
|
|
Stoelting, R.K.,
"Pharmacokinetics and Pharmacodynamics of Injected
and Inhaled Drugs", in Pharmacology and Physiology
in Anesthetic Practice, Lippincott-Raven Publishers,
1999, 1-17. |
Genetic Factors: in
Biotransformation of Drugs
-
Genetic influences: Variation in drug
metabolism rates or in receptor sensitivity:
-
Metabolism:
-
Patients can be categorized as either
rapid or slow acetylators; a classification which refers
to the patients ability to relatively rapidly or slowly
catalyze acetylation reactions. Biotransformation of
some drugs are affected by acetylation rates, examples
include hydralazine (Apresoline) and isoniazid (INH).:
-
Pharmacogenetics: One major concern is that on
underlying disease state may not be appreciated until an
unexpected reaction to an anesthetic agent in fact occurs.
The anesthetic agent essentially exposes on underlying disease
state and then appropriate inner operative responses
required. Examples:
-
Atypical cholinesterase enzyme
suggested by prolonged succinylcholine (Anectine) or
mivacurium (Mivacron)- induced neuromuscular blockade
-
Succinylcholine (Anectine) or volatile
anesthetic induced malignant hyperthermia-Malignant
hyperthermia is a very serious reaction requiring a
definitive treatment approach including dantrolene (Dantrium).
-
If the patient exhibits glucose-6-phosphate
dehydrogenase deficiency certain drugs
may induce hemolysis
-
Barbiturates may induce
intermittent porphyria attacks. It is extremely
important to determine therefore preoperatively if the
patient has history of intermittent porphyria.
Acute intermittent porphyria
|
Background:
-
Porphyria is an inherited condition in which too much of
the chemical porphyrin is synthesized. Porphyrin is used
to make heme, the oxygen-carrying component of blood.
-
Porphyrias are associated with overproduction of
porphyrins and for acute intermittent porphyria the
exacerbation is induced by barbiturates, sulfonamides, and
the antifungal drug griseofulvin.
|
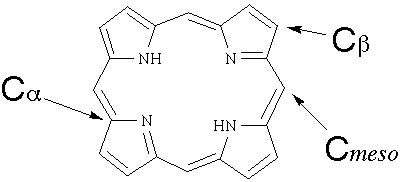
Porphyrin |
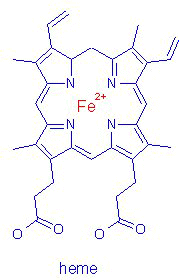
|
-
The specific defect that leads to acute intermittent
porphyria is due to a defect in the specific enzyme called
porphobilogen deaminase (PBG deaminase) also called
uroporphyrinogen synthesis, or HMB synthase, a heme-synthesizing enzyme
-
HMB synthase catalyzes the
conversion of porphobilinogen to hydroxymethylbilane
which is the immediate precursor of uroporphyrinogen
III.
-
In this autosomal dominant
condition (acute intermittant porphyria, there is on
50% normal HMB (hydroxymethylbilane) synthase activity
which results in porphobilinogen buildup.
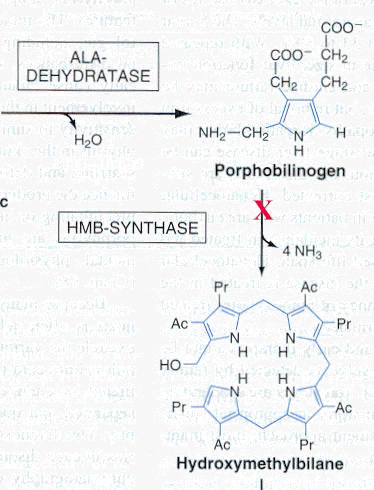
Desnick, Robert J., The
Porphyrias in Harrison's Priniciples of Internal Medicine, (Braunwald,
E., Fauci, A.S. Kasper, D.L., Hauser, S.L., Longo, D.L. and
Jameson, J.L.,eds) 15th Edition, ch. 346, pp
2261-2263.McGraw-Hill, New York, 2001
-
Pathology:
biosynthetic byproducts may turn the urine red and even
can cause, following deposition, reddish brown teeth.
-
Acute episodes of neuropathic syndromes involving
abdominal pain is the most common symptom; Abdominal pain
is typically steady and poorly localized; however,
cramping with ileus, abdominal distention, and reduced
bowel sounds are common. These symptoms are neurologic
rather than inflammatory in origin.
-
Peripheral neuropathy, which may not
occur in all acute attacks, is secondary to axonal
degeneration.
-
CNS symptoms are numerous and in
addition to anxiety, depression, hallucinations, and
disorientation seizures may occur.
-
Paresthesias
& paralysis may occur with even death resulting from
respiratory paralysis. Acute attacks can involve
psychotic episodes and hypertension, and although these
attacks usually do not occur before puberty, they can be
precipitated by barbiturates & sulfonamides which
induces an early but important rate-determining enzymatic
step in heme synthesis, specifically delta aminolevulinic
acid synthesis
-
Other factors known to precipitate acute intermittent
porphyria include alcohol, starvation, infection, and
hormonal changes -- acute intermittent porphyria
exacerbations are more common in females.
-
Clinical management:
-
supportive treatment
-
dextrose infusion
-
high carbohydrate intake
-
hematin infusion (heme), a feedback inhibitor of heme
synthesis (drug may cause renal damage)
-
For management of abdominal pain
associate with acute attacks, narcotic analgesics
may be used and relief from nausea, vomiting,
anxiety and restlessness may be provided by
phenothiazine administration.
-
Safe drugs for use in patients with
acute intermittent porphyria, hereditary coproporphyria
and variegate porphyria:
-
narcotic analgesics,
aspirin,acetaminophen (Tylenol, Panadol),
phenothiazines, penicillin & derivatives,
streptomycin, glucocorticoids, bromides, insulin,
atropine.
-
Unsafe drugs for use in patients
with acute intermittent porphyria, hereditary
coproporphyria and variegate porphyria:
-
barbiturate, sulfonamide antibiotics,
meprobamate (Miltown), glutethimide (Doriden),
methyprylon (Noludar), ethchlorvynol (Placidyl),carbamazepine
(Tegretol), succinamides,carbamazepine (Tegretol),
valproic acid (Depakene, Depakote), griseofulvin,
ergot alkaloids, synthetic estrogens &
progestogens, danazol (Donocrine), alcohol.
-
Prevalence: highest in Sweden, frequency is 1 in 1000
-
Prevalence based on previous manifestation of acute
intermittent porphyria (AIP), about 1 in 50,000; however,
this number probably underestimate the number of
individuals with latent AIP.
Source: National Center for Biotechnology Information
(http://www3,ncbi.nlm.nih.gov/Omim/) (http://www3.ncbi.nlm.nih.gov/htbin-post/Omim/dispmim?176000)
|
|
|
Stoelting, R.K.,
"Pharmacokinetics and Pharmacodynamics of Injected
and Inhaled Drugs", in Pharmacology and Physiology
in Anesthetic Practice, Lippincott-Raven Publishers,
1999, 1-17 |
Influence of Age on Drug
Responses
|
Stoelting, R.K.,
"Pharmacokinetics and Pharmacodynamics of Injected
and Inhaled Drugs", in Pharmacology and Physiology
in Anesthetic Practice, Lippincott-Raven Publishers,
1999, 1-17.
|
Drug-Drug Interactions
-
Definition: Drug interaction -- when one drug
affects the pharmacological response of a second
drug given at the same time.
-
Drug interactions may be
due to:
-
pharmacodynamic effects
-
pharmacokinetic effects
-
Consequences of drug
interactions:
-
Examples
-- positive, beneficial drug interaction effects:
-
propranolol + hydralazine
(reflex tachycardia (undesirable) caused
by hypotensive hydralazine-mediated
response is prevented by
propranolol-mediated b-adrenergic receptor blockade
-
Opioid-induced respiratory
depression may be counteracted by
administration of the opioid receptor
antagonist naloxone
-
Adverse effects -- toxic reactions
-
one
drug may interact with another to impede
absorption
-
one drug may compete with
another for the same plasma
protein-binding sites
-
one drug may affect
metabolism of another by either enzyme
induction or enzyme inhibition
-
one drug may change the
renal excretion rate of the other.
Stoelting, R.K.,
"Pharmacokinetics and Pharmacodynamics of Injected
and Inhaled Drugs", in Pharmacology and Physiology
in Anesthetic Practice, Lippincott-Raven Publishers,
1999, 1-17.
|
Dolin, S. J. "Drugs and pharmacology" in Total
Intravenous Anesthesia, pp. 13-35 (Nicholas L. Padfield, ed), Butterworth
Heinemann, Oxford, 2000
Desnick, Robert J., The Porphyrias in Harrison's
Priniciples of Internal Medicine, (Braunwald, E., Fauci, A.S. Kasper, D.L.,
Hauser, S.L., Longo, D.L. and Jameson, J.L.,eds) 15th Edition, ch. 346, pp
2261-2263.McGraw-Hill, New York, 2001
|